Eskenazi Hospital, formerly Wishard Hospital and City Hospital, is Indianapolis’ oldest hospital. For most of its history, the primary purpose of the city’s public hospital, first known as City Hospital, then Indianapolis General Hospital, Marion County General Hospital, Wishard Hospital, and as of 2013 Eskenazi Hospital, has been to provide health care for the indigent.
The idea of establishing a city-run hospital dates to the 1830s when , a prominent local physician, stressed the need for a permanent place to care for the sick, especially smallpox and cholera victims. Not until 1854, however, did the construction of a hospital building begin. When the facility was completed three years later, the city decided that a hospital was no longer necessary and debated its future.
With the outbreak of the , the city transferred the building to the federal government for use as a hospital for sick and wounded troops. At the war’s end, the federal government gave the hospital building back to the city. In August 1866, the city opened the Indianapolis City Hospital as a 75-bed charity hospital. As with all municipal hospitals, political problems, underfunding, and overcrowding plagued the institution almost from its inception.
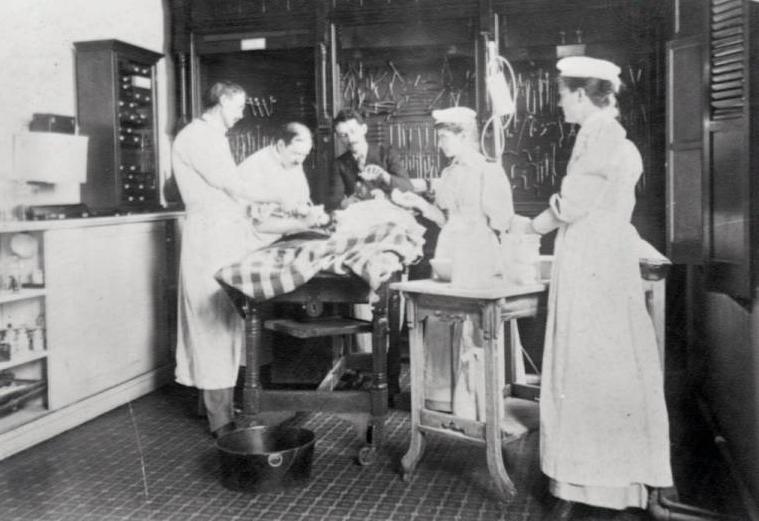
During the late 19th century, the basic character of hospitals changed. Initially viewed as places of last resort for the unwanted of society, they became institutions offering advanced diagnosis and specialty services. At City Hospital, many improvements occurred under the administration of (1879-1886). Wishard obtained money to build additional ward space, established antiseptic procedures, and introduced a trained nursing staff. Various medical schools used City Hospital for teaching purposes (see ).
By the end of the century, the hospital began offering specialty services such as obstetrics-gynecology, ophthalmology, gastroenterology, neurology, and urology. Despite these improvements, the hospital remained overcrowded and lacked adequate space for tuberculosis patients. Not until 1917, when Sunnyside Sanitarium opened, did the hospital have proper facilities to care for those suffering from tuberculosis.

City Hospital’s constant overcrowding resulted from both chronic underfunding and its duty to care for a disproportionate share of the city’s sick, poor, and all of the city’s African American population. In the 1920s and 1930s, it was the only hospital in the city to care for the Black community. Because the hospital lacked proper funding and because of prevailing prejudices, the care of Black patients at the institution was often inferior.
Despite these problems, City Hospital witnessed a number of improvements during the 1920s, including the relocation of the City Dispensary to the hospital (see ), which gave the institution an outpatient department. The hospital also constructed a new surgery unit. In 1929, the hospital received a $50,000 anonymous donation to establish a clinical research laboratory. The laboratory was run by .
The most significant improvements in the hospital’s history occurred during the administration of Dr. , who served as superintendent from 1931 to 1951. Myers was instrumental in securing the appointment of Black hospital staff and the opening of new wards for Black patients in 1939. He was also responsible for the purchase of the first iron lung, the opening of the first municipal cancer clinic, improved care for tuberculosis patients through the construction of Hospital (1936), and new facilities for psychiatric patients. Increasing costs associated with modern medicine meant that the hospital could no longer rely exclusively on tax money for all of Myer’s improvements. From the 1930s onward, the institution looked to philanthropy to fund a number of major improvements (see ).
In 1947, Myers changed the name of the hospital from the Indianapolis City Hospital to Indianapolis General Hospital. In 1959, the name changed to Marion County General Hospital to reflect the broader base of the population served by the institution. After his retirement as superintendent, Myers served on the board of directors where he continued to spearhead change, such as the opening of the Krannert Institute of Cardiology in 1963. He served on the board until 1968.
The hospital’s name was not the only thing to change during this time. By the late 1940s, the hospital ceased being governed by the Board of Health and Charities. In 1951, a new governing body, the , was created to remove the hospital from political influence and to provide better care for the city’s residents.
Despite the improvements introduced by Myers, his tenure was not without problems. After the construction of new patient wards in 1939, Myers was unable to gain approval for any more construction projects until 1962. Moreover, World War II took its toll on the hospital. Approximately 50 percent of the active staff was called for military duty.
Conditions became so bad that in 1956 the appointed a citizens’ committee to investigate the situation. They concluded that the nursing board, the executive director, and the superintendent failed to communicate with each other, and the hospital lacked adequate equipment and supplies and suffered from insufficient funding and undue political influence.
Not until the 1960s were major changes undertaken to rectify the hospital’s problems. Sunnyside Sanitarium and General Hospital merged in 1961, and the next year the hospital undertook a $16 million expansion. In 1969, the hospital entered into a formal agreement with Indiana University allowing faculty of the school to share joint appointments at Indiana University and at General Hospital.
By the 1970s, the hospital had 726 beds and numerous outpatient clinics. To offer better services and consolidate its efforts, in 1975 the hospital opened the , which had been substantially funded by the donations of Eli Lilly and Company and the Regenstrief family. Emphasis during these years was on improved service. Psychiatric care was offered both on the wards and at the Midtown Community Mental Health Center.
Delivery of services, however, was hindered by an image problem. Because the hospital was viewed exclusively as a charity hospital, its care was believed to be inferior, and it had trouble attracting pay patients. To overcome this problem, the hospital changed its name in 1975 to Wishard Memorial Hospital and allowed Indiana University to manage the facility. Although the hospital remained a separate legal entity, it became a functional component of the . The hospital also established a burn unit (1977) and became known for its treatment of trauma cases.
In the 1980s, skyrocketing medical costs and the hospital’s obligation to care for the county’s indigent and uninsured patients placed severe financial strains on Wishard. In 1988, a report commissioned by the hospital board (known as the Pettinga report) noted that the hospital provided a major service to the community and to the medical school. For those reasons, the commission recommended that the hospital seek more compensation from city and state governments to fulfill its original mission.
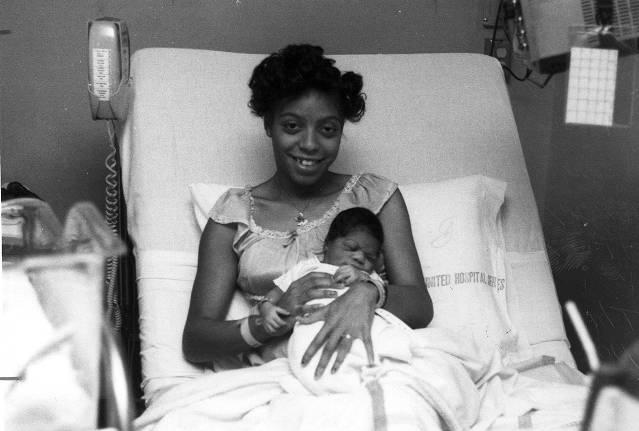
Lack of sufficient outpatient clinics to serve the community, an image problem, high Black infant mortality, overcrowding, and the lack of funding remained problems in the 1990s. The decade was not, however, an entirely bleak one. The fiscal affairs of the hospital improved with the increase of support from federal programs such as Medicare and Medicaid, as well as private insurance coverage.
Several new programs were added to the hospital as well. In 1992, Wishard became the first verified Level 1 trauma center in Indiana. In 1995, HHC also opened its first skilled nursing facility, Lockefield Village, to provide long-term care on the Wishard campus. The Wishard Advantage Program served needy residents in , and Wishard Senior Care was launched in 1997. A year later, a 24-hour nursing triage system, Health Connection, began operation, and the Acute Care for Elders Unit was established. In 1999, the IU National Center of Excellence in Women’s Health opened at Wishard, an Emergency Medicine department was created, and the Palliative Care Program was launched.
By the 2000s, Wishard was serving two-thirds of the uninsured hospital patients in Marion County making it one of the busiest hospitals in the state. It also had a $77 million deficit in 2002 due in part to the rise in the cost of uncompensated care. In an effort to rectify the substantial deficit by 2005, several measures were taken to cut costs and raise money over the course of three years.
To cut costs, the hospital began working with Indiana and Medicaid officials, encouraged the use of lower-cost pharmaceuticals, sent bills out 30 days sooner, reduced labor through voluntary severance packages, and reduced the number of full-time positions. The hospital worked to increase revenue by training employees to properly identify all procedures for better insurance reimbursement rates and by adding more procedures that could be performed at the hospital, including bariatric surgery. Wishard also opened the Burn Center in 2003 to replace the original unit.
In 2003, under the leadership of HHC president Matt Guttwein, HHC began purchasing nursing homes not only to improve long-term care but also to improve agency finances and help Wishard. The reimbursement policies of the federal-state Medicaid program allowed HHC to pay the state Medicaid agency extra fees that triggered higher federal matching funds. While he stated that improving care at nursing homes was HHC’s priority, Guttwein also admitted in 2011 that the policy helped boost HHC’s overall finances and helped it expand services at Wishard, a move made necessary in part by inadequate local funding.

The end of the early 2000s initiated the end of an era for Wishard. In 2009, a referendum passed with 85 percent approval for a new hospital to be constructed a half-mile west of the old facility. The ground-breaking for the $754 million project took place in May 2010. A year later, Wishard received a $40 million donation, the largest gift in its history, from Sidney and Lois Eskenazi to help build the new hospital. In recognition of this gift, the hospital was renamed the Sidney & Lois Eskenazi Hospital.
The project not only created thousands of jobs but also engaged primarily Indiana businesses–particularly minority, women, and veteran-owned business participation. After four years, the new 316-bed inpatient and 200-bed outpatient facility was complete. The Sidney & Lois Eskenazi Hospital opened on December 7, 2013, at 720 Eskenazi Avenue.
The new building brought in new features for healing and wellness. In 2014, the Common ground plaza and Sky Farm rooftop garden opened. These outdoor green spaces were created to provide staff, patients, and the community spaces of beauty for contemplation, wellness, and healing. In addition, Eskenazi became the first hospital in the nation to seek Leadership in Energy and Environmental Design (LEED) certification, which it was awarded in 2015.
Early in 2020, the HHC came under fire after an investigation revealed that Indiana received more supplemental Medicaid nursing home funding than any other state and alleged that those monies had not been used appropriately. The investigation stated that a 2016 report compiled by American Senior Communities (the firm hired to manage the HHC-owned facilities) claimed that 25 people had defrauded HHC nursing homes of at least $35 million but only five individuals were prosecuted and $15.5 million recovered. The agency reputedly had been using a provision of Medicaid funding policies to divert reimbursements from nursing homes to other projects, including the construction of the Sidney & Lois Eskenazi Hospital. This occurred over the previous two decades and totaled over $1 billion.
The 2020 Novel Coronavirus (COVID-19) pandemic heightened attention to problems in HHC long-term care facilities. Between March and August, the first six months of the pandemic, HHC nursing homes accounted for about 23 percent of COVID-19 deaths in such facilities although it owns about 11 percent of them in the state.
These numbers raised more questions about how shifting money from nursing homes to Eskenazi Hospital and other programs had affected them and their ability to respond to such crises. In August 2020, Guttwein resigned, succeeded by Paul Babcock, who had been public health and safety director in the , as interim president.
The Sidney & Lois Eskenazi Hospital is the main campus of the Eskenazi Health system, which includes 10 sites that provide health services throughout the Indianapolis community. In 2020, Eskenazi Hospital treated more COVID-19 patients than any other hospital in the state.
In August 2022, ASC agreed to pay $5.5 million in a settlement over allegations that it submitted false claims to the federal Medicare program. Babock made it clear that Eskenazi and HHC were not a party in the lawsuit and that the municipal corporation had taken steps to improve oversight“ requiring American Senior Communities to adhere to a comprehensive compliance plan.”

Help improve this entry
Contribute information, offer corrections, suggest images.
You can also recommend new entries related to this topic.